-
Original Article
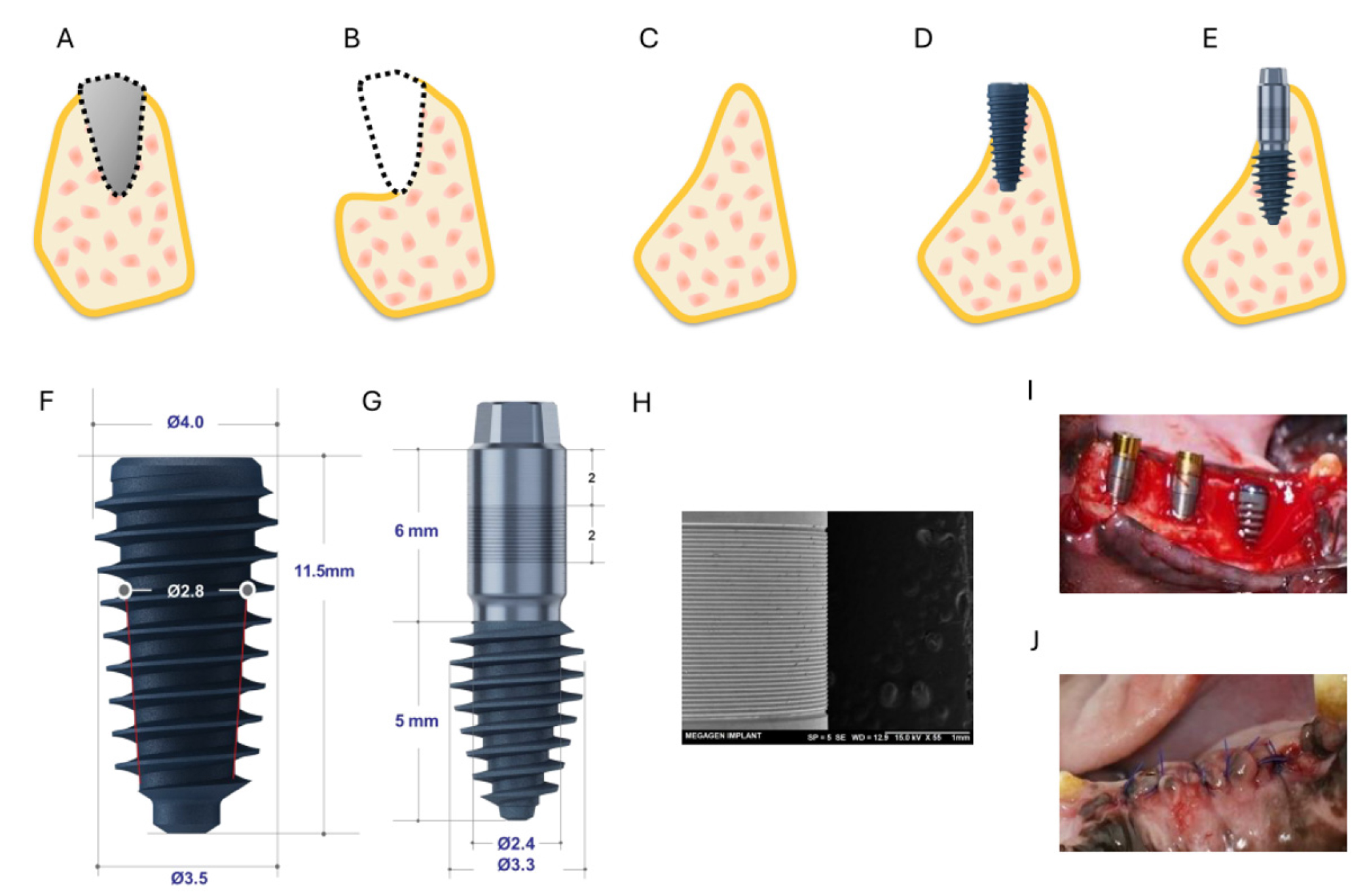
- Early Hard- and Soft-tissue Response to a Novel Long-cuff Implant with a Microgrooved Neck Surface: A Proof-of-concept Study
- Donghyun Lee, Jungwon Lee, Young-Chang Ko, Ki-Tae Koo, Jordi Gargallo-Albiol, Cristian Dinu, Hyun-Wook An, Ji-A Jung, Kwang Bum Park
- Purpose: This proof‑of‑concept animal study evaluated the early hard- and soft-tissue responses to a novel long-cuff implant that incorporates a long, machined …
- Purpose: This proof‑of‑concept animal study evaluated the early hard- and soft-tissue responses to a novel long-cuff implant that incorporates a long, machined neck with a microgrooved surface. Materials and Methods: Six beagle dogs received both conventional (control) and novel long-cuff (test) implants in the mandible following a 2‑month healing period after tooth extraction. Each animal was fitted with one control implant and five test implants, randomly distributed across three sites on each side of the mandible. Radiological and histological assessments were performed at 2, 4, and 6 weeks. Outcome measures included inflammatory response, bone volume/tissue volume (BV/TV), bone‑to‑implant contact (BIC), bone area (BA), soft‑tissue attachment, and collagen density. Results: Both implant types exhibited comparable inflammatory patterns, peaking at 4 weeks and resolving by 6 weeks. BV/TV remained stable over time (control: 17.89 ± 5.06%; test: 20.18 ± 2.25% at 6 weeks). At 6 weeks, the microgroove surface demonstrated greater soft‑tissue attachment (85.98 ± 20.64%) and collagen density (25.12 ± 13.64%) than the machined surface (62.76 ± 28.03% and 14.14 ± 9.56%, respectively) and the control group (69.42 ± 13.15% and 19.70 ± 4.40%, respectively). BIC and BA followed similar trajectories in both groups; at 6 weeks, BIC reached 18.27 ± 0.34% in controls and 15.90 ± 14.08% in the test group. Conclusion: The novel long-cuff implant elicited biological responses comparable to those of conventional implants while promoting enhanced soft‑tissue attachment and collagen deposition at the microgrooved region. This design may represent a viable alternative for atrophic ridges that would otherwise require bone augmentation. - COLLAPSE
-
Original Article
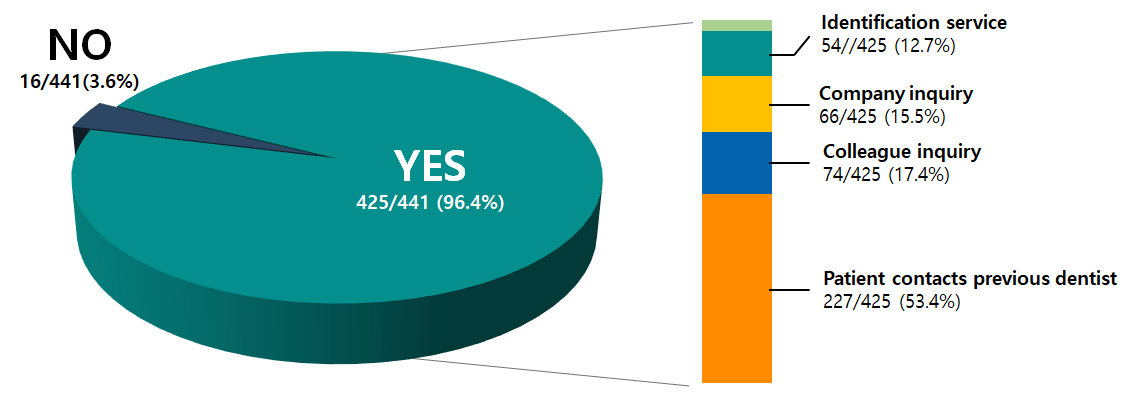
- Dentists’ Experiences with Unknown Implant Systems and Acceptance of Artificial Intelligence-based Identification Tools
- Sanghoon Park, Yiseul Choi, Hyun Jin Park, Jong-Ki Huh, Wonse Park
- Purpose: Dental implant use has increased substantially in South Korea. However, clinicians often encounter patients with unknown implant systems. Identifying implant systems …
- Purpose: Dental implant use has increased substantially in South Korea. However, clinicians often encounter patients with unknown implant systems. Identifying implant systems is essential for maintenance and complication management. Existing methods are fragmented, and empirical data on information-seeking patterns and acceptance of AI-based tools are limited. This study examined dentists’ experiences with unidentified implant systems, strategies used to obtain missing information, awareness and use of manual identification services, and willingness to adopt AI-based identification tools.Materials and Methods: A cross-sectional online survey was conducted among licensed dentists in Korea (n = 500). The questionnaire collected information on implant practice patterns, experience with unidentified fixtures, information-seeking methods, awareness and use of manual expert-based identification services, and willingness to use an AI-based identification system.Results: Among the respondents, 96.4% (425/441 respondents who performed implant surgery) reported having encountered cases in which the implant system could not be identified. The most common method for obtaining information was asking patients to contact their previous dentist (53.4%), followed by consulting a colleague (17.4%), contacting the implant company (15.5%), and using a manual identification service (12.7%). Awareness and use of manual identification services were each 36.0%. Most respondents (64.0%) indicated that they could not identify the implant systems on radiographs. Willingness to adopt an AI-based identification tool was high (96.2%), with the largest proportion of “Yes” responses among dentists in their 40s.Conclusion: Unknown implant systems pose challenges in clinical practice. Dentists rely on multiple informal strategies to obtain missing information. Limited awareness of existing services, combined with a strong willingness to adopt AI-based tools, underscores the need for more accessible and efficient implant information support systems. - COLLAPSE
-
Clinical or Case Report
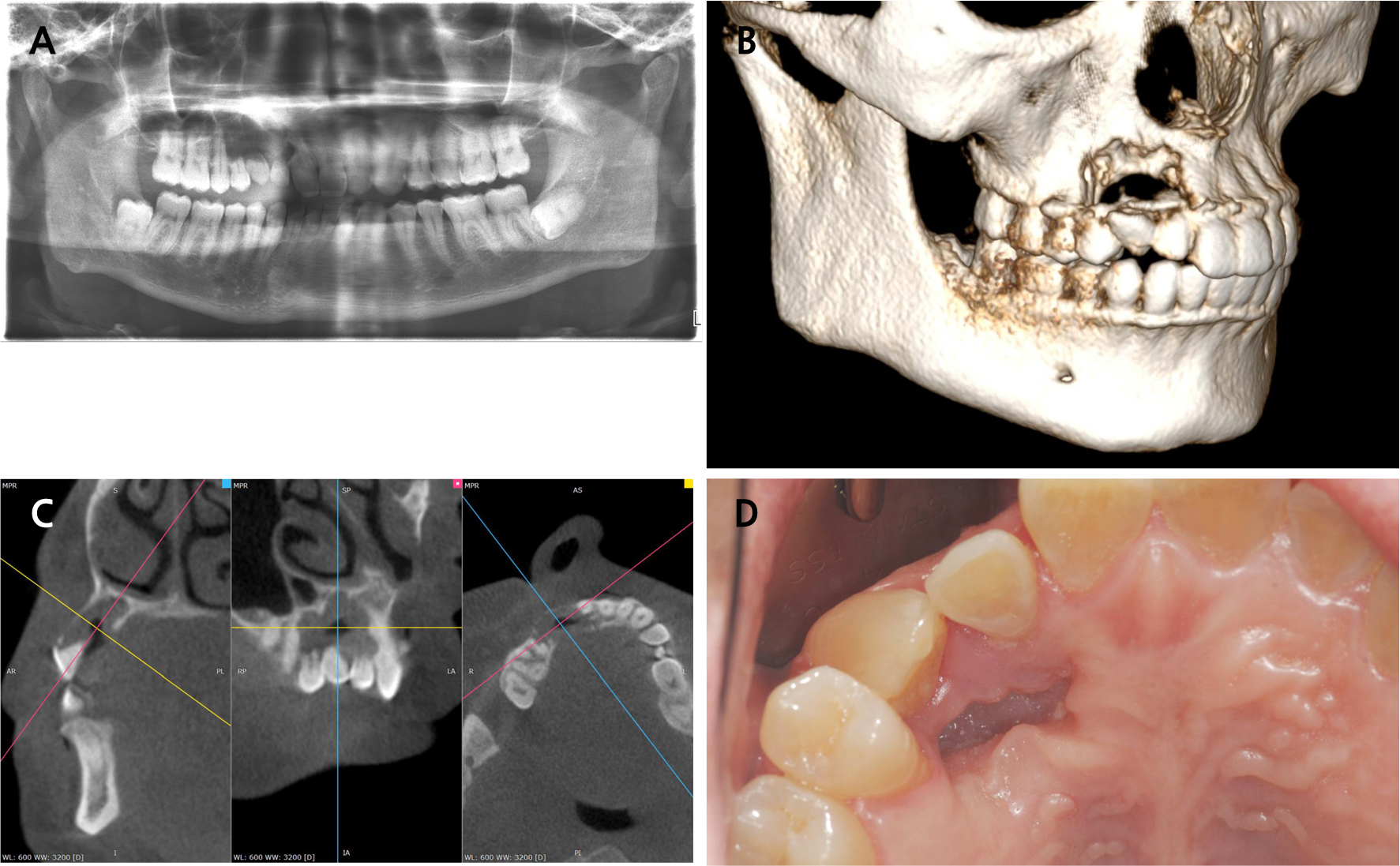
- Successful Ramal Bone Grafting for Maxillary Defect Following Chemical Burn Injury
- Ahjin Kim, Jin-yong Cho
- Long-term sequelae of chemical burns in oral cavity can result in severe alveolar bone defects. This case report presents a patient who …
- Long-term sequelae of chemical burns in oral cavity can result in severe alveolar bone defects. This case report presents a patient who was 40 years previously burnt with sulfuric, and developed multiple root resorption and a palatal segmental bone defect in the right maxillary anterior and premolar regions without any pathological lesions. Surgical intervention involved the extraction of hopeless teeth (#12, #13, #14), elevation of the palatal soft tissue as a flap, and reconstruction using autogenous ramal cortical bone combined with an allogenic bone graft and covered with a resorbable membrane. Following the healing period, two dental implants were placed at positions 13 and 14 , and a three-unit fixed dental prosthesis was delivered. Complete bone regeneration was achieved and maintained over a 3-year follow-up period. The implants demonstrated excellent stability and satisfactory aesthetic and functional outcomes. Radiographic examination confirmed complete osseointegration and volume stability of the grafted area. This case showed that ramal cortical bone when combined with allogenic bone and covered by healthy palatal tissue, can successfully reconstruct segmental alveolar defects. The use of indigenous palatal soft tissue as a covering flap has proven to be critical for achieving predictable bone regeneration and long-term volume stability. - COLLAPSE
-
Clinical or Case Report
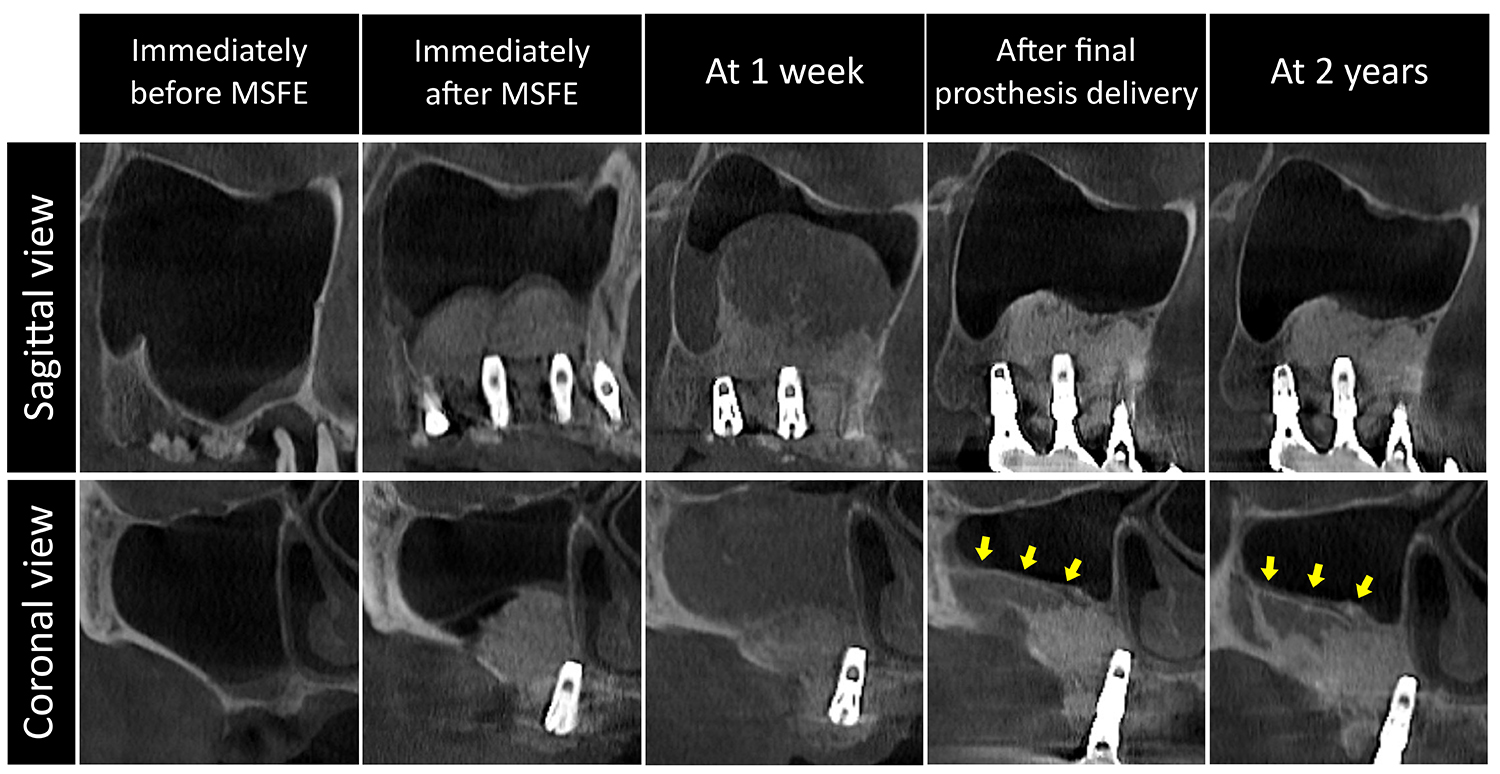
- Unexpected Spontaneous Bone Formation Beyond the Boundary of the Grafted Area Following Lateral Maxillary Sinus Floor Augmentation: A Report of Four Cases
- Won-Bae Park, Gyutae Kim, Young Woo Song, Seungil Shin, Hyun-Chang Lim
- Maxillary sinus floor elevation (MSFE) is a common procedure to address insufficient bone height in the posterior maxilla for implant placement. In …
- Maxillary sinus floor elevation (MSFE) is a common procedure to address insufficient bone height in the posterior maxilla for implant placement. In MSFE, bone substitute grafting is commonly employed to create space for new bone formation, which is typically confined to the grafted area. Conversely, this case study demonstrates unexpected spontaneous bone formation (SBF) beyond the grafted region. In four patients, lateral MSFEs with or without simultaneous implant placement were performed. Sinus membrane perforation was not detected during MSFE. Cone-beam computed tomography (CBCT) was obtained pre-operatively, at 1 week, at prosthesis delivery, and during follow-up. Early CBCT revealed significant sinus mucosal swelling and varying graft particle dispersion, without clinical signs of infection. Subsequently, new bone formed beyond the grafted region, particularly along the lateral sinus wall, with progressive maturation and cortical thickening. All implants achieved functional stability. These findings suggest that post-operative events such as bleeding, transient mucosal thickening, or possible undetected membrane perforation may create additional space beyond the grafted area, which subsequently undergoes bone formation. The clinical impact of SBF may be limited, but it provides insight into the osteogenic potential of the sinus environment. - COLLAPSE
-
Clinical or Case Report
- Rehabilitation of a Severely Atrophic Maxilla Using Sinus Augmentation and Palatal Rotational Flap for Implant-retained Overdenture: A Case Report with Literature Review
- Sanghoon Lee, Kyong-Seop Lee, Kyoungsik Yoon
- Rehabilitation of a severely absorbed maxilla poses significant surgical and prosthetic challenges owing to limited bone availability, sinus pneumatization, and insufficient keratinized …
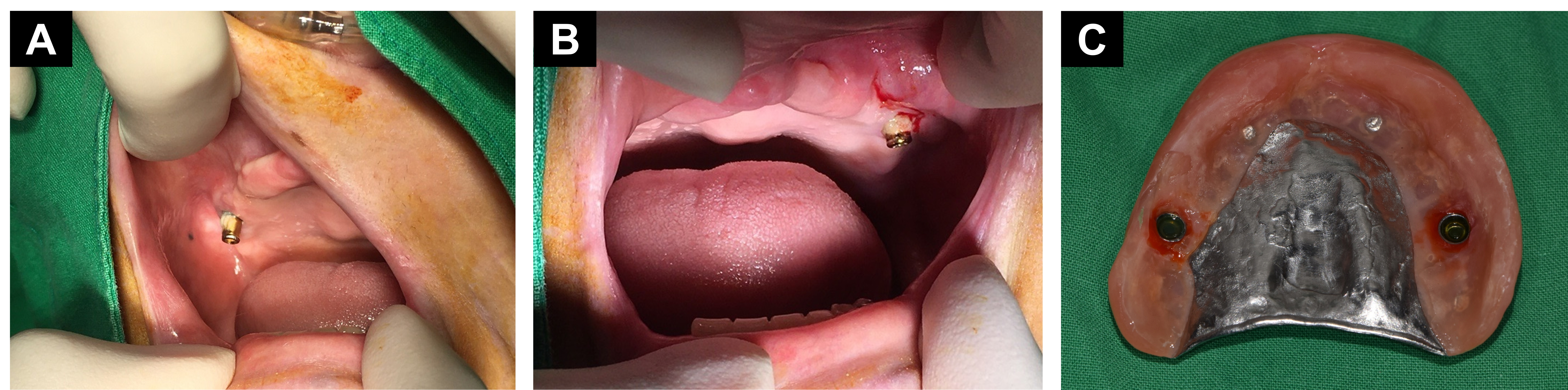
- Rehabilitation of a severely absorbed maxilla poses significant surgical and prosthetic challenges owing to limited bone availability, sinus pneumatization, and insufficient keratinized mucosa. Implant-retained overdentures (IROD) offer a less invasive and cost-effective alternative to fixed prostheses; however, compromised bone and soft tissue conditions often necessitate complex reconstructive procedures. This case report describes the staged management of a 70-year-old woman who presented with spontaneous exfoliation of the maxillary implants for overdenture support. Following the removal of the residual fixtures, bilateral sinus augmentation via the lateral window technique was performed with a freeze-dried cortical bone allograft, enabling the placement of four wide-diameter implants in the posterior maxilla. In second-stage surgery, the extremely shallow vestibular depth precluded the use of conventional free gingival grafts. Instead, bilateral palatal rotational flaps based on the greater palatine artery were used to augment the keratinized mucosa around the abutments. This approach resulted in stable peri-implant soft tissue, satisfactory prosthetic retention, and the absence of mucosal irritation. Although posterior-only implant placement is inherently accompanied by biomechanical limitations, such as anterior cantilevering, this report highlights the feasibility of combining sinus augmentation and palatal rotational flap techniques for clinically favorable IROD rehabilitation in patients with extreme maxillary atrophy. - COLLAPSE
Journal Informaiton
 Journal of implantology and applied sciences
Journal of implantology and applied sciences
Journal Informaiton
Journal Informaiton - close
 Journal of implantology and applied sciences
Journal of implantology and applied sciences













