Ⅰ. Introduction
Restoration of an edentulous maxilla remains a complex challenge in implant dentistry, particularly in the presence of advanced alveolar ridge resorption. An atrophic maxilla is typically characterized by limited bone volume, particularly in the posterior region, owing to pneumatization of the maxillary sinuses, low bone density, and residual ridge atrophy. These conditions can severely compromise the dental implant placement, primary stability, and long-term prognosis of implant restorations.1,2
Beyond the challenges of hard tissue reconstruction, the soft tissue environment surrounding implants plays a pivotal role in long-term peri-implant conditions and prosthetic longevity. Adequate keratinized mucosa (KM) facilitates oral hygiene, reduces soft tissue inflammation, and improves patient comfort during implant restoration. Researchers have introduced various surgical procedures to preserve or enhance peri-implant KM, including apically positioned flap combined or not with vestibuloplasty, autogenous free gingival graft (FGG), split-thickness skin graft, palatal rotational flap and allogenic or xenogeneic soft tissue graft.3,4
Implant-retained overdentures (IROD) are a practical and less invasive option for edentulous maxilla with insufficient bone volume for multiple dental implants with standard dimensions and an adequate alveolar bone span for rehabilitation. IROD are commonly supported by 2–4 dental implants, providing enhanced retention over conventional complete dentures while minimizing the need for extensive grafting procedures.5,6 IROD can be designed using various attachment systems, including bars, studs, and magnet attachments, and has demonstrated favorable clinical outcomes in terms of patient satisfaction, masticatory performance, and oral hygiene maintenance.7 Despite slightly lower survival rates than implant-supported fixed prostheses,8 IROD offer significant advantages in terms of cost-effectiveness, surgical simplicity, and maintenance access, particularly in medically compromised or older patients.9
This case report describes the comprehensive management of a patient with severe maxillary atrophy who presented with discomfort due to an implant-retained overdenture. A staged treatment plan involving bone augmentation, implant placement, and KM augmentation was implemented. The present case highlights the challenges and considerations in hard and soft tissue management for IROD in a severely resorbed maxilla and discusses the clinical rationale and limitations of this approach.
II. Case Report
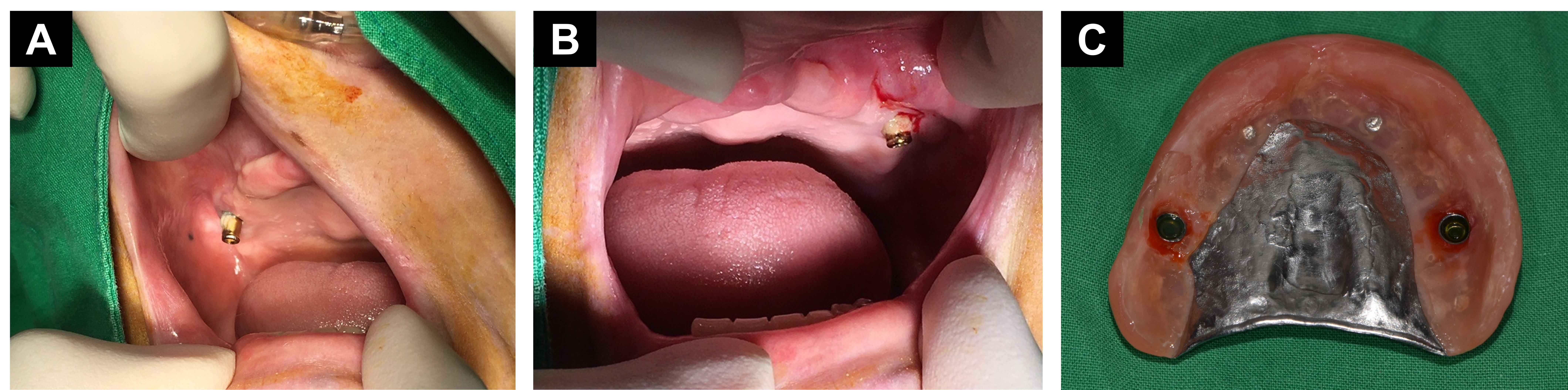
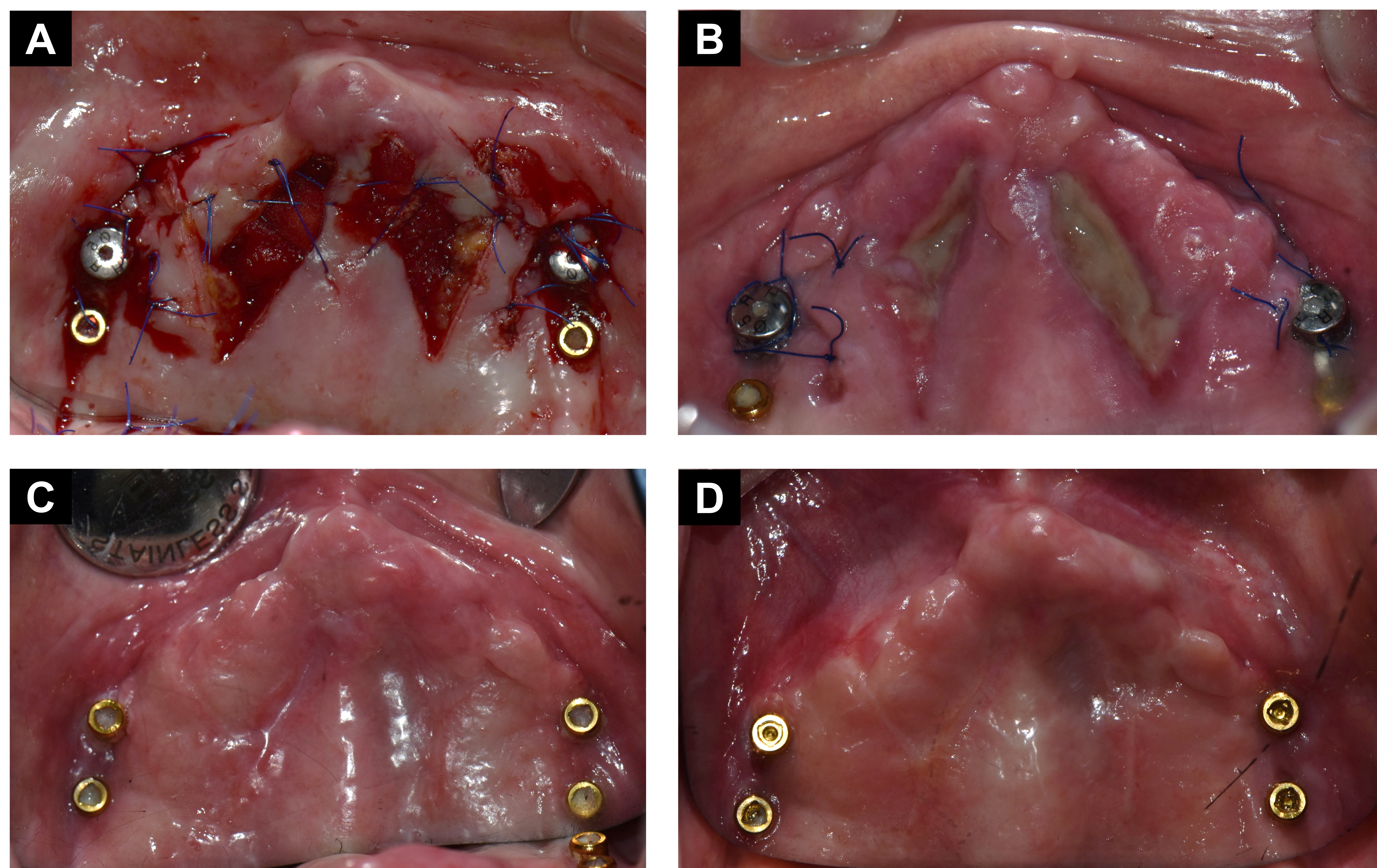
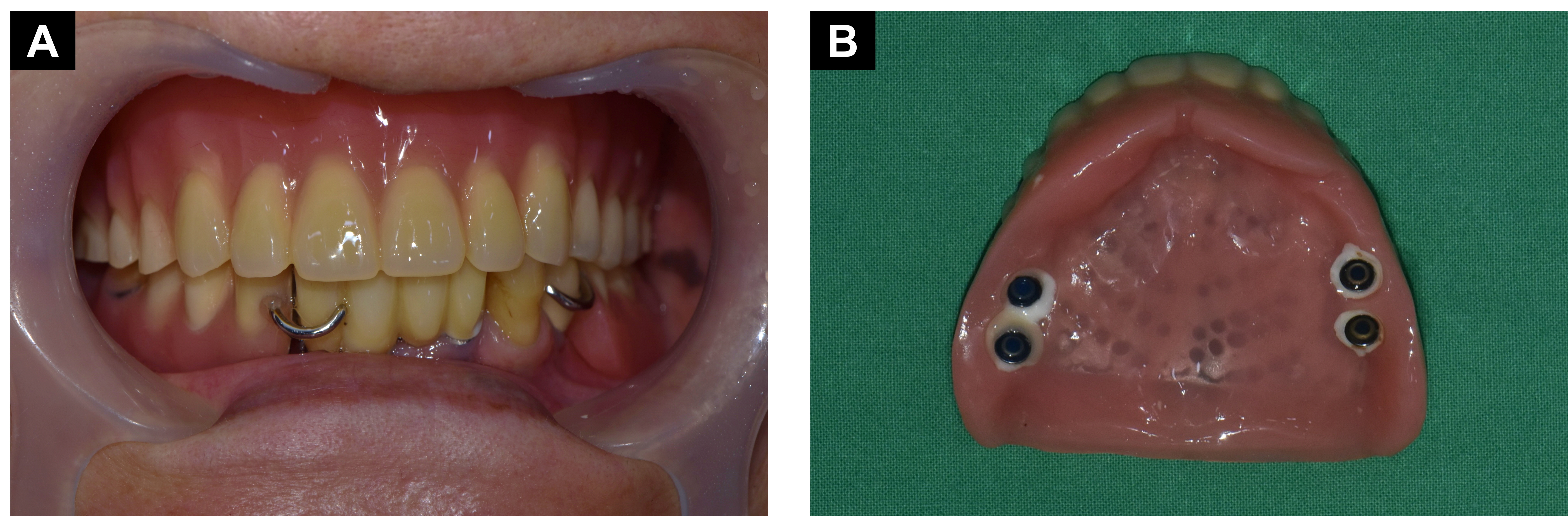
A 70-year-old woman visited the Department of Oral and Maxillofacial Surgery for rehabilitation of the maxilla following the occurrence of pain and swelling in bilateral dental implants for overdentures. Upon clinical examination, severe vertical and horizontal alveolar bone resorption was observed, and the remaining implant attachment was positioned within the vestibule. Nonkeratinized gingiva surrounded the locator attachment (Fig. 1A and 1B). A previous IROD were fabricated and retained by a dental implant on each side of the maxilla. Owing to its long-term use, the denture exhibited poor adaptation and irritation caused by tissue impingement (Fig. 1C).
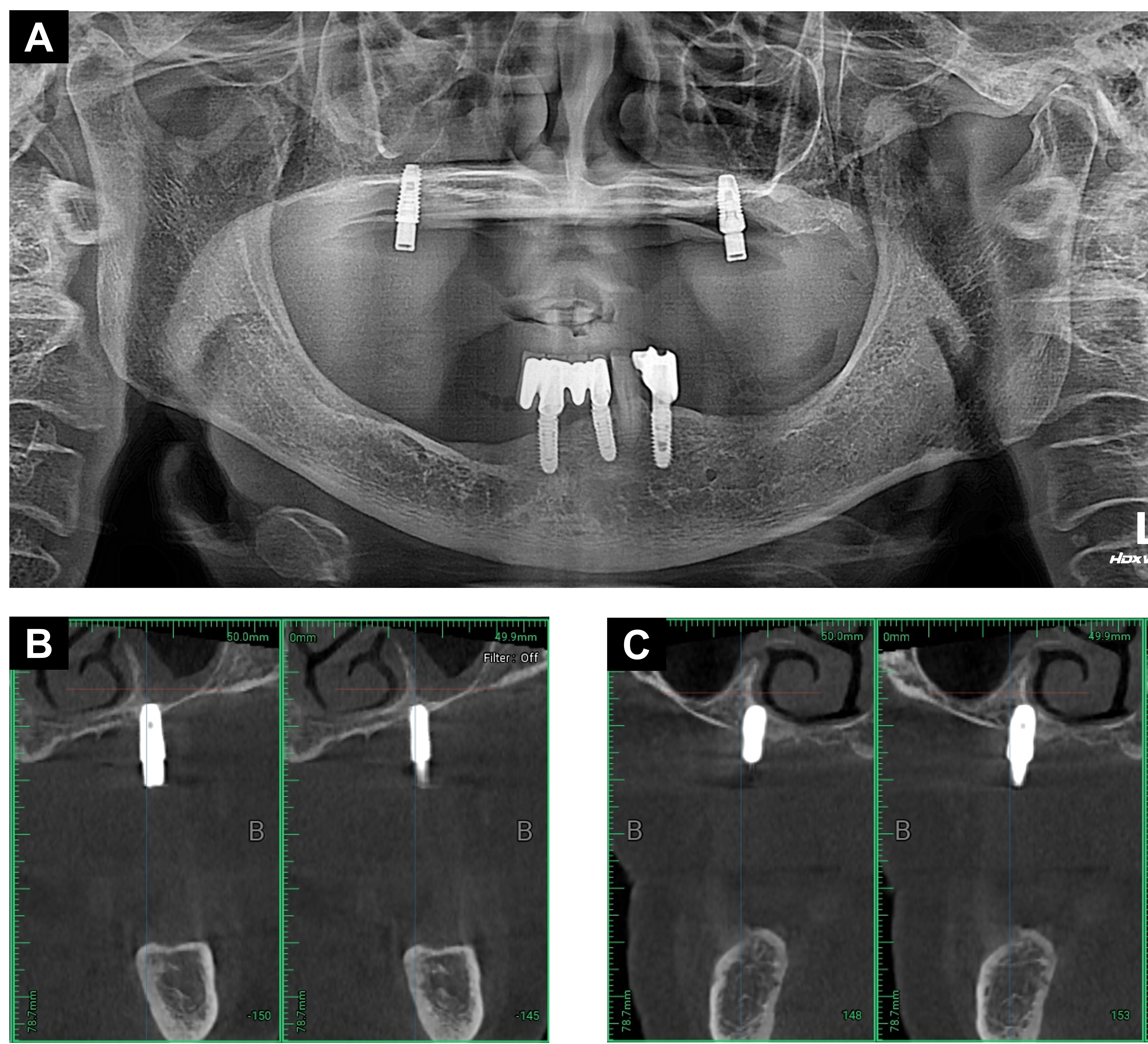
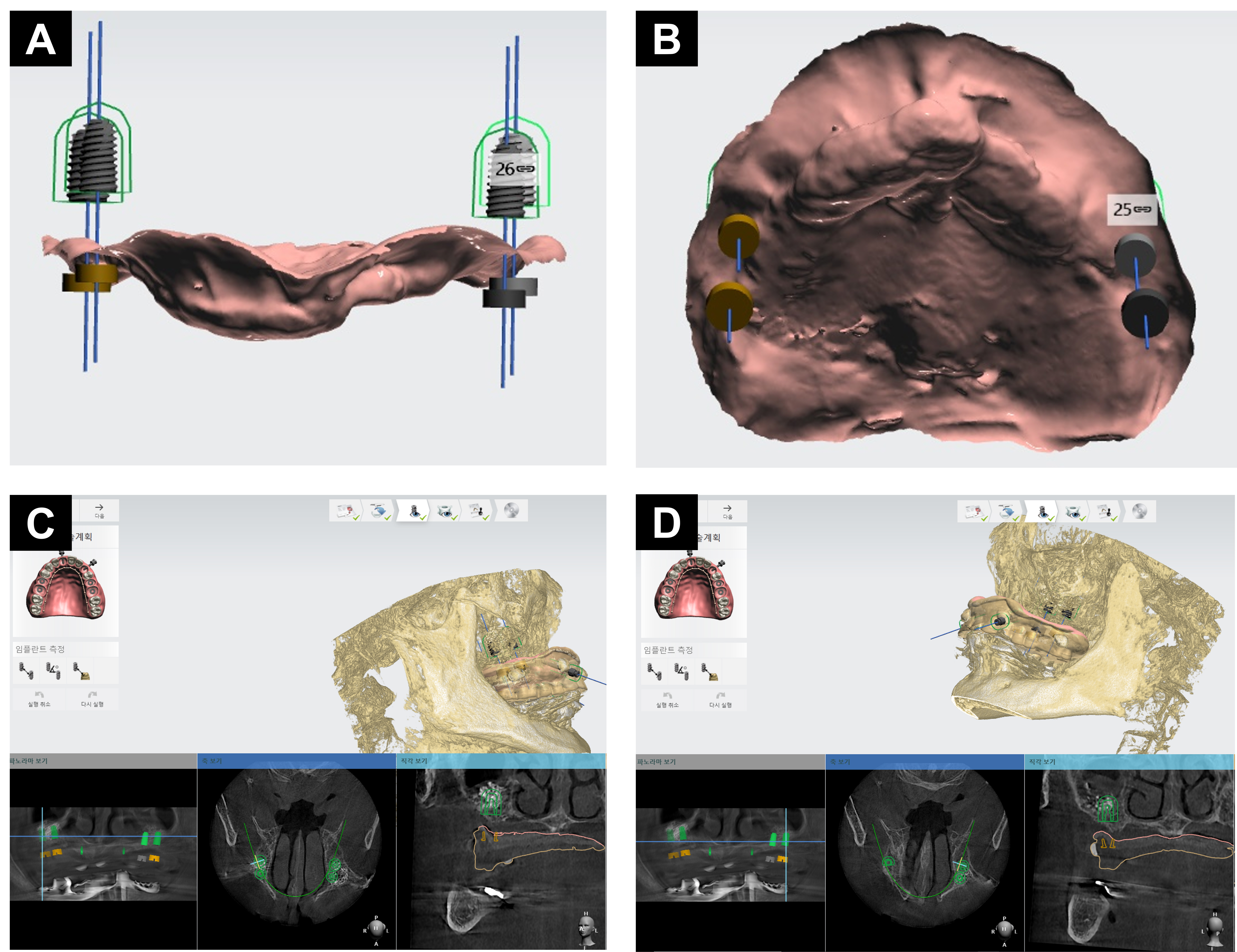
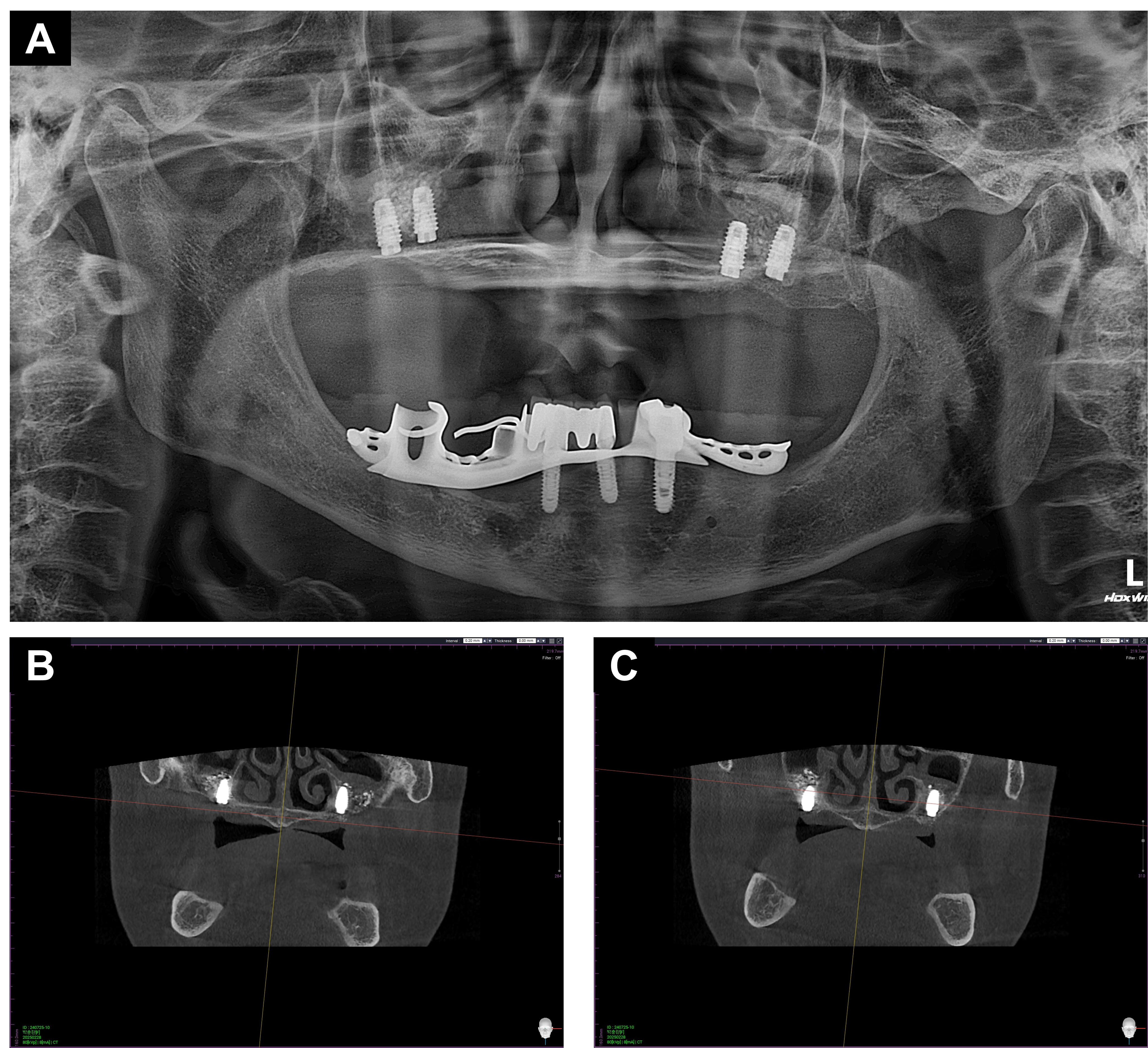
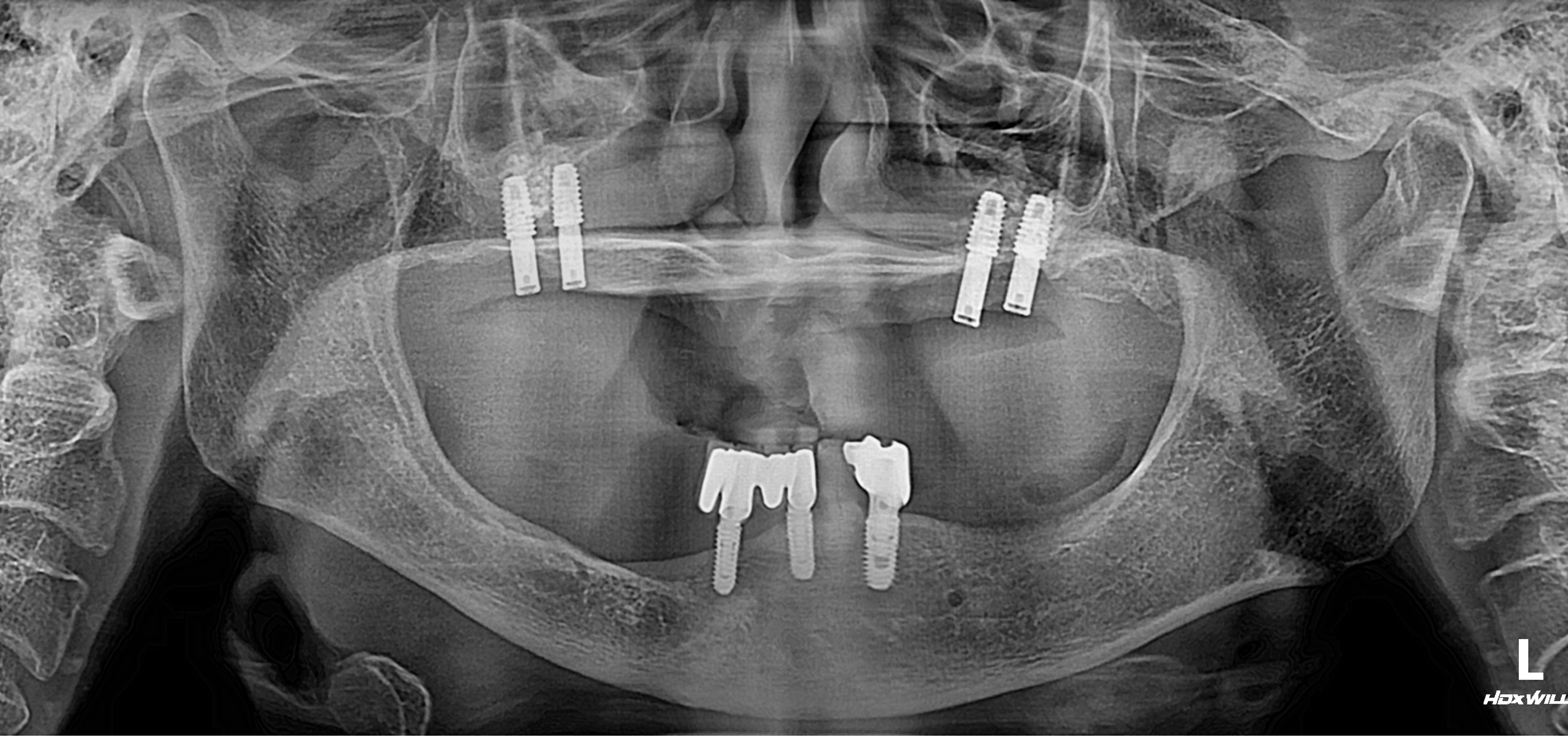
Radiographic examination revealed extreme vertical and horizontal atrophy and advanced marginal bone loss at the residual fixtures of the dental implants in the bilateral posterior maxilla (Fig. 2). After intraoral scanning, an implant-retained overdenture was planned, and to achieve predictable bone augmentation, the placement of the implant fixture was determined in the molar area. The surgical plan was established using computer-aided design software (Implant Studio; 3Shape, Copenhagen, Denmark) (Fig. 3). Compared with previously placed fixtures, the path of implantation was determined to be toward the maxillary sinus rather than toward the nasal cavity. Under intravenous conscious sedation with conventional local anesthesia, removal of residual fixtures and simultaneous bone augmentation in bilateral sinus augmentation via lateral window (SALW) was performed using a freeze-dried cortical bone allograft (SureOss; HansBioMed, Seoul, Korea). The SALW procedure was performed using a conventional transoral antrostomy technique as described in a previous study.10 At 6 months after SALW, dental implants with a diameter of 5.0 mm and a length of 8.5 mm (SM II UV fixture; Point Implant, Gyeonggi, Korea) were placed on bilateral maxillary molar area, respectively (Fig. 4). In the second stage of surgery, performed 3 months later, an apically positioned flap, including approximately 2 mm of attached gingiva, was created in conjunction with a healing abutment connection. Following gingival healing, even a 9-mm-long healing abutment was partially covered, particularly on the mesial aspect of the anterior healing abutment, owing to buccal mucosal impingement (Fig. 5A). Considering the extremely shallow vestibular depth, an apically positioned flap combined with a conventional free gingival graft is considered inadequate. As a substitute, bilateral palatal rotational pedicle flaps based on the greater palatine artery were elevated to augment the KM at the mesial region of the healing abutments on each side. Additionally, the buccal flaps involving the palatal KM at the distal end were elevated and distally repositioned at the buccal region of the healing abutments (Fig. 5B and 5C). Four weeks after flap rotation, augmented KM around the anterior healing abutment was confirmed, and impressions were obtained for the definitive implant-retained overdenture (Fig. 6A to 6C). Following delivery of the definitive prosthesis, no notable soft tissue irritation around the dental implants was observed, as an adequate width of augmented KM was maintained around the attachments (Figs. 6D and 7). Follow-up panoramic radiography showed stable marginal bone levels in the implants (Fig. 8).
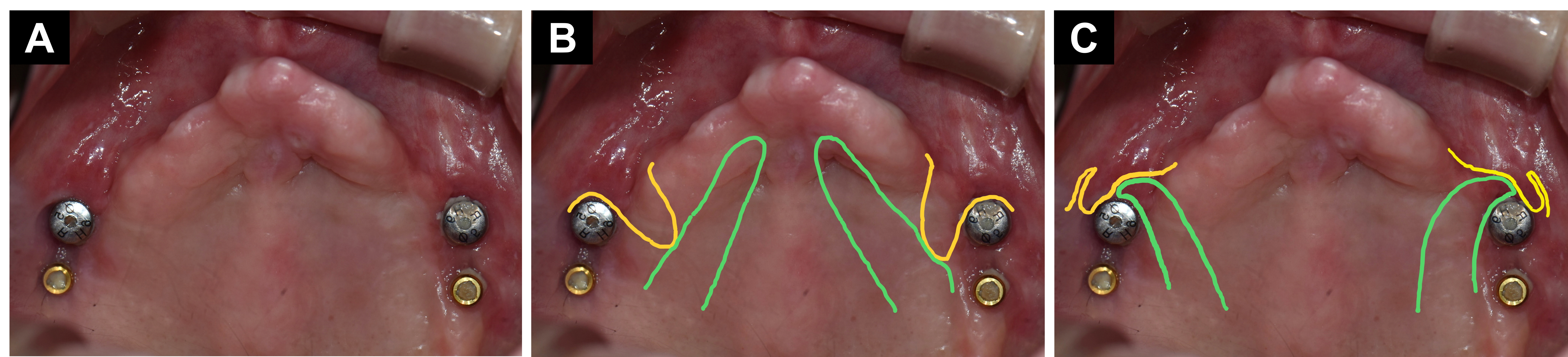
Fig. 5.
Clinical photograph after healing abutment connection. (A) Insufficient keratinized mucosa around the mesial healing abutment, (B) schematic design for raising a palatal rotational flap, (C) schematic design for the inset of the flap. (The green and yellow lines indicate the palatal rotational pedicled flap and the buccal flap that is repositioned distally, respectively.)
III. Discussion
Oral rehabilitation with dental implants at previously failed sites and in extremely atrophic maxilla has long been considered a considerable clinical challenge. Severe atrophy of the maxilla not only reduces the quantity and quality of available alveolar bone but also complicates implant placement. Moreover, extensive bone grafting procedures using autologous bone are not always feasible considering the patient’s general condition, surgical burden, prolonged healing period, and donor site morbidity. Repeated surgical interventions may also compromise tissue resilience and flexibility, interfere with further procedures, and reduce predictability. In the present case, the anterior and posterior alveolar bones demonstrated severe resorption down to the basal bone, corresponding to class IV edentulous jaws according to Cawood and Howell11 and the posterior atrophic maxilla system class IV by Zaninovich and Drago.12 In cases where extensive bone grafting in the anterior region is planned, securing a donor site that can provide a sufficient amount for autogenous block bone grafting is challenging. To predict surgical outcomes, conventional dental implants accompanied by SALW were placed in the molar region.
To overcome the extreme limitations of the maxillary anatomy, alternative implant modalities that utilize maxillofacial buttresses, such as the frontal process of the maxilla, zygomatic bone, or pterygoid plate, have been introduced. Zygomatic implants provide a reliable option for patients with severe posterior maxillary atrophy by anchoring them to the zygomatic bone, thus eliminating the need for sinus grafting and enabling immediate loading. Previous studies have reported long-term survival rates exceeding 95% over 5 years, even in severely resorbed maxilla.13,14 Similarly, pterygoid implants bypass the maxillary sinus by engaging the dense cortical pterygoid plate of the sphenoid bone. Since its introduction by Tulasne in 1989, anatomical and radiological studies have recommended a minimum length of 13 mm for adequate anchorage.15 Finally, transnasal implants placed in the frontal process of the maxilla have been described as a salvage option that offers stable anterior anchorage. When combined with zygomatic implants for posterior support, transnasal implants may provide biomechanical advantages by reducing the anterior cantilever forces in full-arch rehabilitation.16 Nevertheless, these modalities demand specifically established surgical and prosthetic expertise with corresponding facilities compared with conventional alveolar implants, limiting their application to carefully selected cases.
In the present case, from a soft tissue perspective, severe resorption of the alveolar ridge down to the basal bone restricted the use of an apically positioned flap for vestibular deepening. Therefore, keratinized gingiva augmentation using a FGG in the deep vestibular area at the depth of the zygomaticomaxillary suture region is considered to have unpredictable outcomes. Therefore, although invasive, a palatal rotational flap based on the greater palatine artery was selected to augment the mesiobuccal area of the anterior overdenture attachment. Consequently, a combined buccal and palatal flap approach was employed instead of the conventional apically positioned flap or FGG. On the buccal side, a laterally repositioned flap of partial thickness was harvested from the palatal mucosa, whereas on the palatal side, a full-thickness rotated pedicle flap based on the greater palatine artery was elevated from the hard palate mucosa.
The palatal rotational flap, which is widely used in oropharyngeal reconstruction or oroantral fistula closure, is associated with significant donor site morbidity and can provide an abundant supply of KM when applied with careful case selection. This flap can be designed in either a unilateral or bilateral configuration, with dimensions exceeding 10 cm2, allowing its application in the reconstruction of extensive oropharyngeal defects. Pedicled flaps have a significantly higher survival rate (approximately 95%) than random-pattern flaps.17 Previous studies have described postoperative complications including intraoperative and postoperative bleeding, sensory disturbances, and flap bulging.13,18 In the present case, the patient did not exhibit any notable complications and demonstrated a favorable healing course. This modality represents a salvage option in cases where conventional soft tissue management is inadequate.
In the present case, bone augmentation was only feasible in the molar regions because of the anatomical configuration of the maxillary sinus, which inevitably encompassed implant placement in the posterior region. Consequently, prosthetic rehabilitation of the maxilla is hindered by the presence of an anterior cantilever, which is an inherent limitation of this approach. Dental implants placed solely in the posterior region are associated with a higher risk of prosthesis rotation and anterior dislodgement owing to the absence of anterior support.14 These biomechanical disadvantages may lead to increased mechanical complications and reduced long-term prosthetic stability, particularly when non-splinted attachments such as locators or balls are used.15 Previous studies have reported higher stress concentrations and lower retention values in posterior-only configurations,16 implying that this strategy should be limited to specific indications and implemented with caution. In conjunction with splinted bar attachments, improved rotational stability has been reported in unfavorable dental implant positions.19
Ⅳ. Conclusion
Within the limitations of this case report, we demonstrated the clinical course of managing hard and soft tissues for implant-retained overdentures in a severely atrophic maxilla. To achieve predictable hard- and soft-tissue augmentation followed by dental implant maintenance, SALW and placement of bone-level implants with an internal connection system were performed in the posterior region. Augmentation of the KM was performed by raising the palatal rotational flaps bilaterally, which resulted in favorable clinical outcomes.